Scientists in the US are working on a new approach to treating kidney failure that could one day free people from needing dialysis or having to take harsh drugs to suppress their immune system after a transplant.
The researchers, based at University of California San Francisco (UCSF), have shown for the first time that kidney cells, housed in an implantable device called a bioreactor, can survive inside the body of a pig and mimic several important kidney functions.
The biorector can work quietly in the background, like a pacemaker, and does not trigger the recipient’s immune system to go on the attack.
The findings are an important step forward for The Kidney Project, which is jointly headed by UCSF’s Shuvo Roy, PhD (technical director) and Vanderbilt University Medical Center’s William H. Fissell, MD (medical director).
Eventually, researchers plan to fill the bioreactor with different kidney cells that perform vital functions like balancing the body’s fluids and releasing hormones to regulate blood pressure – then pair it with a device that filters waste from the blood.
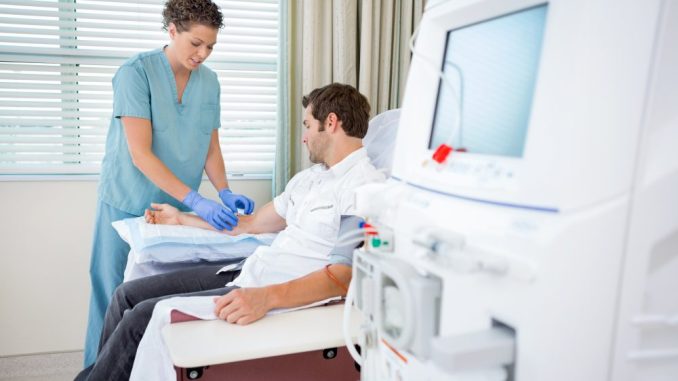
The goal is to produce a human-scale device to improve on dialysis, which keeps people alive after their kidneys fail but is a poor substitute for having a real working organ.
More than 500,000 people in the US require dialysis several times a week.
Many patients seek kidney transplants, but there are not enough donors, and only about 20,000 people receive them each year.
An implantable kidney would be of huge benefit
Roy, a bioengineering professor in the UCSF School of Pharmacy, said:
“We are focused on safely replicating the key functions of a kidney.
The bioartificial kidney will make treatment for kidney disease more effective and also much more tolerable and comfortable.”
The researchers engineered the bioreactor to connect directly to blood vessels and veins, allowing the passage of nutrients and oxygen, much like a transplanted kidney would.
Silicon membranes keep the kidney cells inside the bioreactor safe from attack by the recipient’s immune cells.
The scientists used a type of kidney cell called a proximal tubule cell, which regulates water, as a test case.
Co-author H. David Humes, MD, of the University of Michigan, had previously used these cells to help dialysis patients in the intensive care unit with life-saving results.
The researchers tracked the kidney cells and the recipient animals for seven days after transplantation and both did well.
The next step will be month-long trials, as required for by the FDA, first in animals and eventually in humans.
Roy said:
“We needed to prove that a functional bioreactor will not require immunosuppressant drugs, and we did.
“We had no complications and can now iterate up, reaching for the whole panel of kidney functions at the human scale.”
